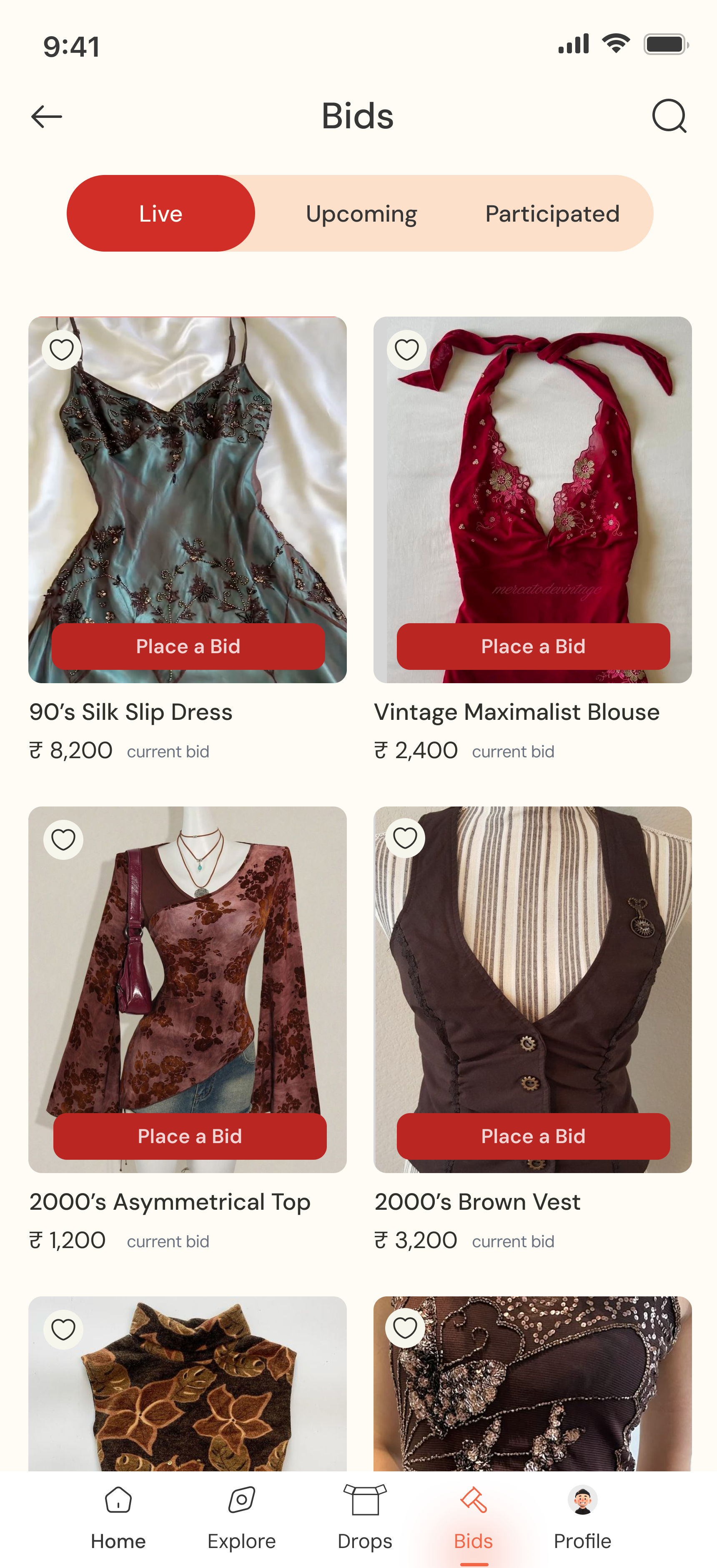
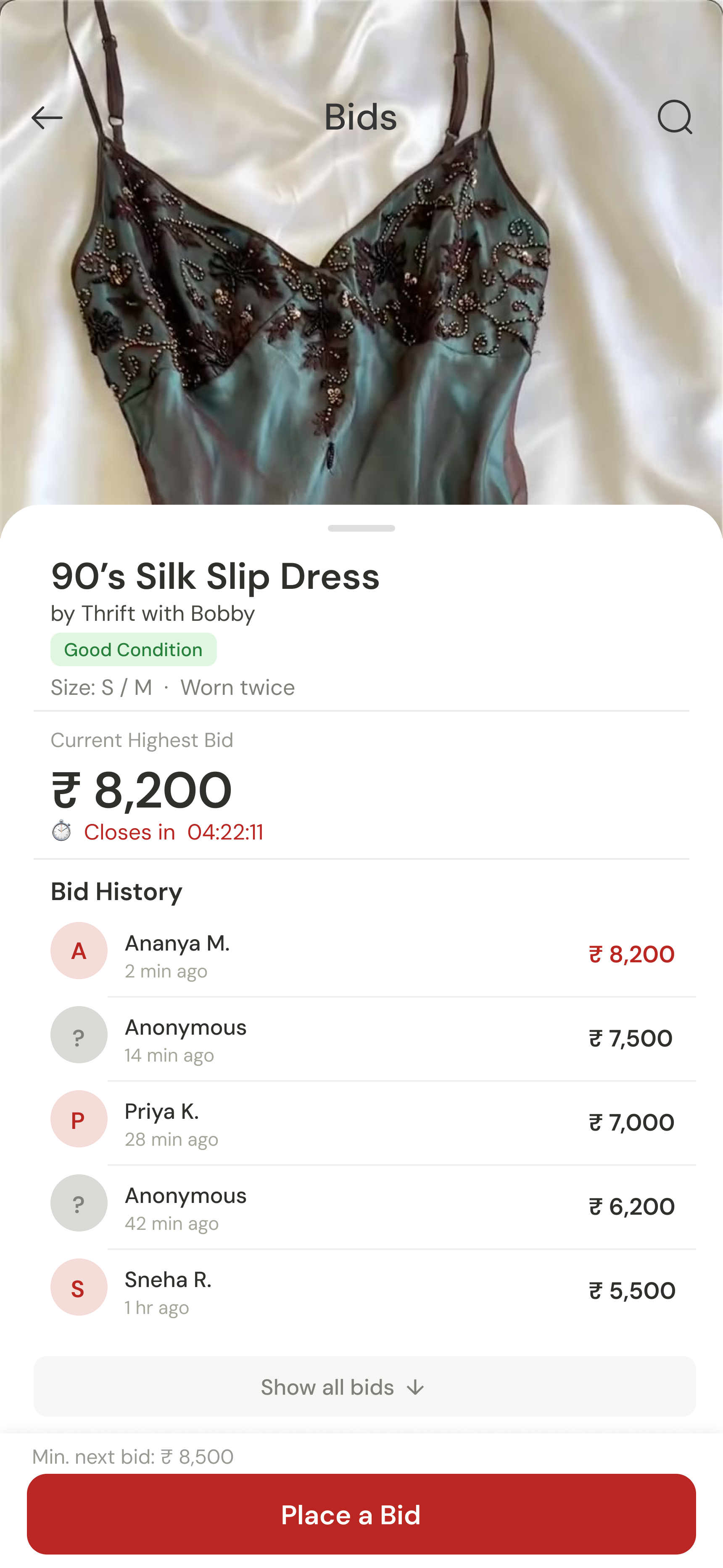
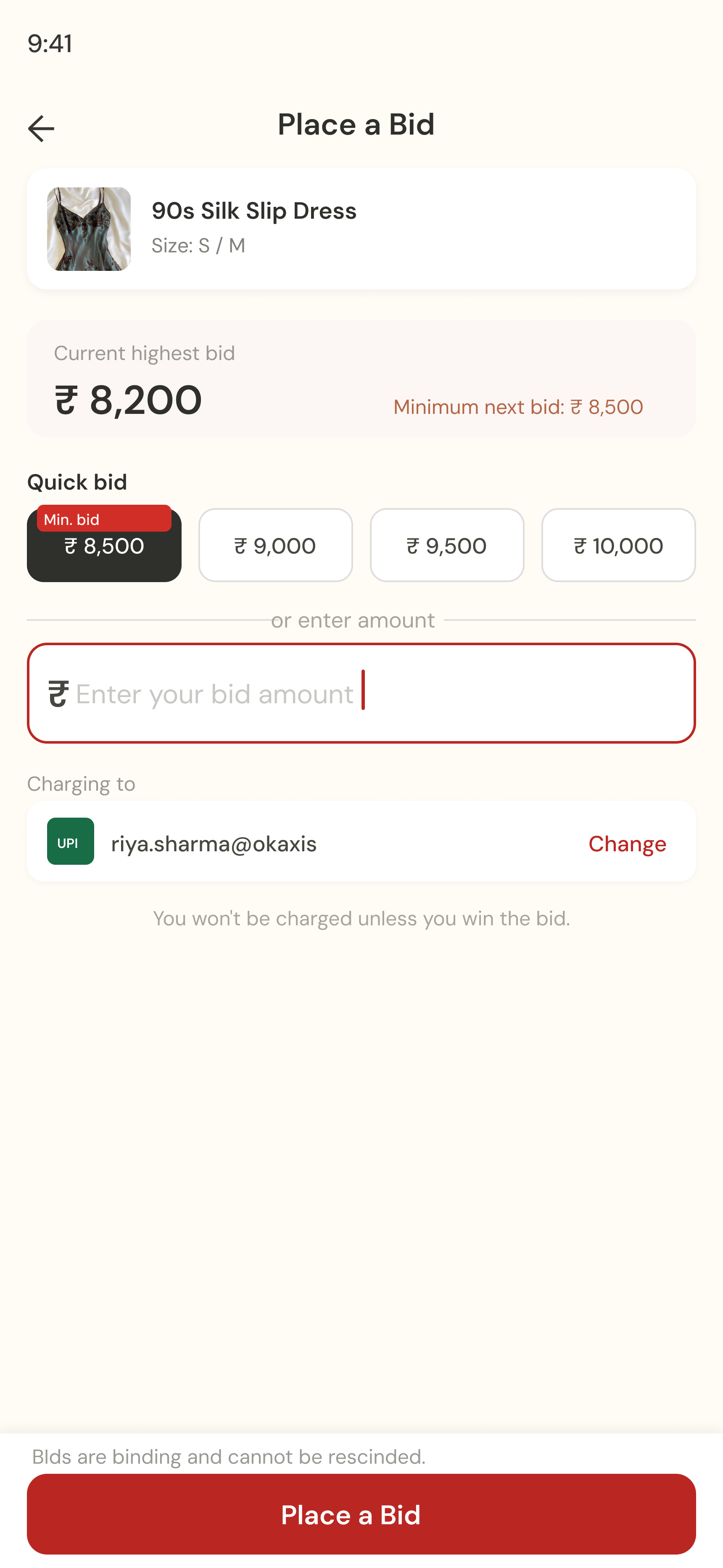
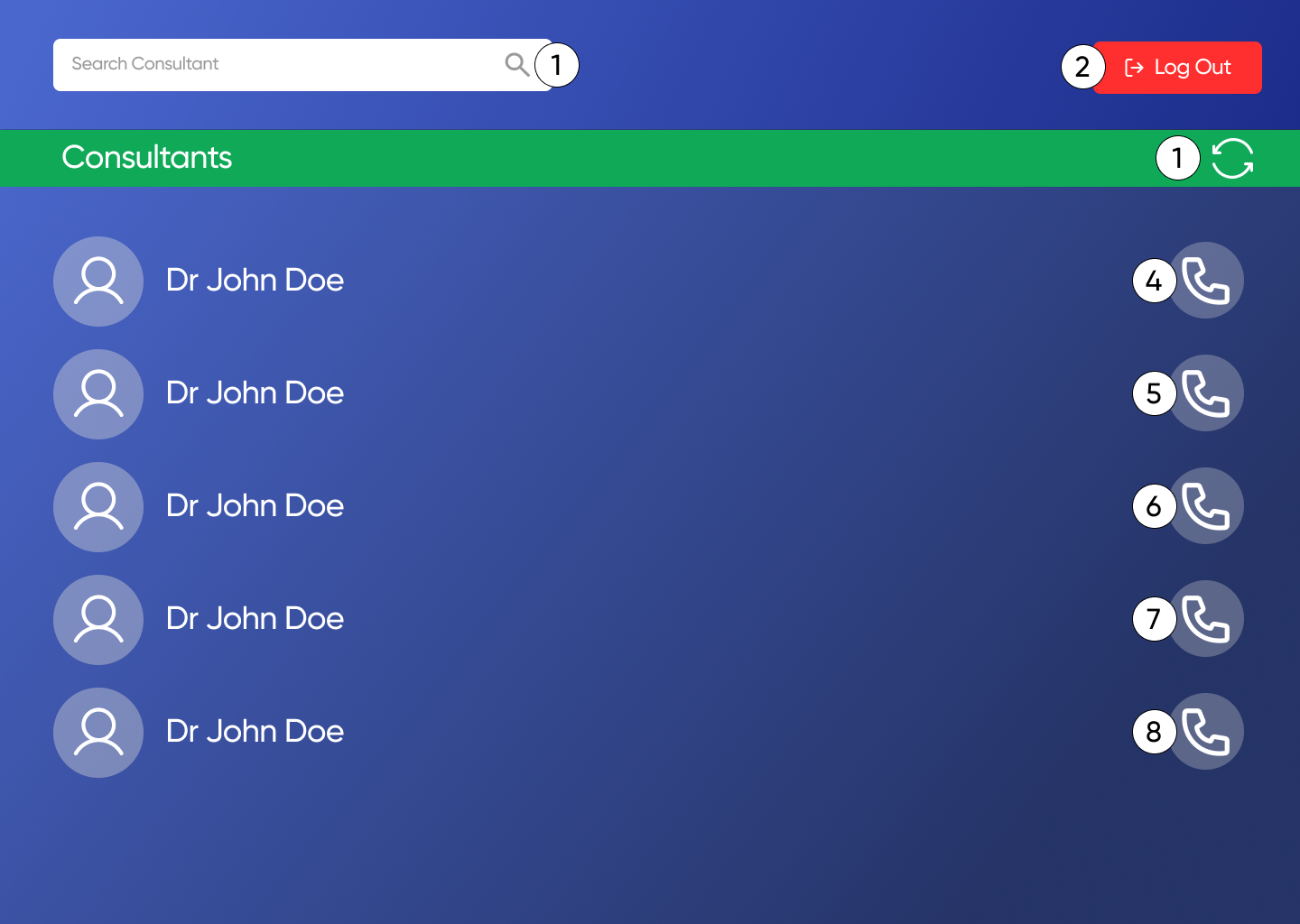
Before any screens were designed, the brand had to exist. Thrift My Drip isn't a neutral marketplace, it has a personality rooted in Indian Instagram drop culture: loud, playful, a little chaotic, and genuinely warm. The visual identity had to reflect that.
The colour palette, Statement Red, Golden Hour, Lemon Pop, Faded Tag, and Closet Black, was built around the energy of a drop moment. Statement Red carries urgency and excitement. Golden Hour and Lemon Pop bring the warmth of thrift-haul aesthetics. Faded Tag references worn labels and vintage provenance. Closet Black anchors everything.
Typography combines three typefaces: Newbery Sans Pro for headlines (structured but friendly), Lust for editorial moments (adds editorial tension), and Gopher for body text (legible and approachable). Together they create a system that can be loud when it needs to be and calm when clarity matters.
Supporting motifs, starbursts and elliptical patterns, were drawn from vintage sale signage and Indian bazaar aesthetics. Applied to social media templates, they give sellers a consistent visual vocabulary without constraining their individual voice. The system was designed to be handed off: sellers should be able to use it without a designer present.